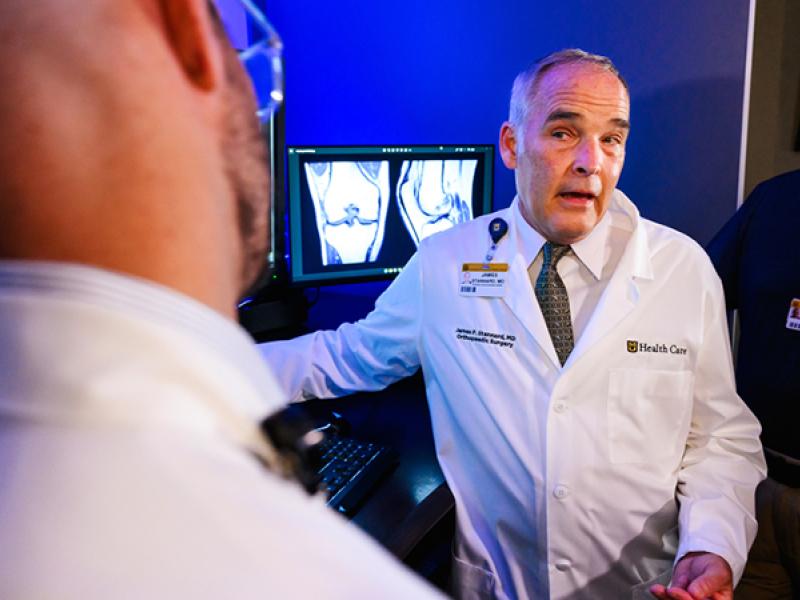
When patients need fractures repaired and wounds sutured in University Hospital's emergency room, the anesthetic of choice is propofol. But no matter how experienced a health care provider is, optimal dosing is tricky.
“You can make ballpark estimates of how much somebody needs, but the way we do it now is you take a syringe and start giving it to them until they get where you want, and then you kind of estimate when they’re going to wake up and re-dose them, because each patient metabolizes and redistributes the drug differently,” said John Yanos, MD, of the Department of Emergency.
Yanos knew there must be a way to improve the initial dosing and maintain an optimal dose during the procedure to reduce the likelihood of human error. In fact, researchers in Europe have created mathematical formulas that predict the appropriate dosage for patients based on their individual characteristics.
Yanos had clinical expertise but could not make sense of the mathematics, much less how to translate the math into a method and computer program that governed the pump. That’s where Peter Tonellato, PhD, the director of the MU School of Medicine’s new Center for Biomedical Informatics, came in handy.
“John provided a collection of papers with models and handed them over and said, ‘I don’t really know what these describe, but I think they’re pertinent,’ ” Tonellato recalled. “I said, ‘This collaboration and project is perfect for us.’ ”
The CBMI’s purpose is to connect medical researchers who have problems to solve with quantitative specialists across campus who are experts in areas such as math, statistics, computer science and engineering. By tapping the collective brain power of the entire campus, MU medical researchers are more likely to create projects that lead to publications, grants and, most important, improved patient care.
The CBMI, located across the hall from the School of Medicine's J. Otto Lottes Health Sciences Library, is designed to be welcoming and collaborative. Floor-to-ceiling windows allow passers-by to see what’s going on inside. As the space was being redesigned, Tonellato requested all walls be removed so the interior was open and conducive to multidisciplinary collaborative “palavers.”
“The palavers — or forums — are pretty novel,” Tonellato said. “They’re not just lectures. There are tons of lectures. Quantitative people lecture at the School of Medicine and medical scientists from the School of Medicine lecture to engineers, mathematicians and statisticians. That approach on its own does not create a connection. You attend the lecture, and it’s very exciting, but what comes next?
“The forums CBMI launched have a collection of people from the departments you would like to engage. They participate in an assessment of a problem being presented. The purpose of the participants in the forum is defining and clarifying the problem through writing a multi-page scientific statement on the problem, including a scientific hypothesis and therefore objectives and a sense of how you might approach those objectives. That process and statement are the beginning of a multidisciplinary collaborative project.”
The idea for the CBMI began with Eduardo Simoes, MD, the chair of the Department of Health Management and Informatics, and Jerry Parker, PhD, the associate dean of research. They thought modern precision medical research required better collaboration between the medical and informatics fields. Patrick Delafontaine, MD, the dean of the MU School of Medicine, agreed.
“We’ve had an exponential increase in the data we get from all sources, including the patients themselves,” Delafontaine said. “One of the key challenges in health care is to analyze this data, sort it and try to see what is more important and what is less important so we can actually make better-informed decisions. We have in Dr. Tonellato a real expert in biomedical informatics who participated in and started similar programs at Harvard, The Medical College of Wisconsin and the University of Wisconsin.”
The CBMI fits into the University of Missouri’s larger initiative to build the Translational Precision Medicine Complex. The goal of that program is to create a home for multidisciplinary collaborative research on disease treatment and prevention that accounts for the physiological, genetic, environmental and lifestyle differences in individual patients.
Yanos’ propofol project is a perfect example.
The research team includes doctors and nurses collecting the data on the clinical side, two experts in mathematical modeling, two data analysts and a genetic counselor.
The math and data specialists are validating the European mathematical models against information collected from MU Health Care patients. If the results correlate, the health informatic computer experts of the Tiger Institute will write and integrate the code that regulates the pumps to deliver a baseline amount of the anesthetic that doctors could adjust slightly as needed.
As Yanos pointed out, if a formula could determine the right continuous dose of anesthetic, the same could be done with antibiotics or any other drug, which will lessen the possibility of errors and improve patient outcomes. And the groundwork is being done using what Tonellato calls “clinical avatars” — virtual patients.
“The nice thing about informatics is you don’t have to have a bench lab to do this,” said Matt Robinson, MD, the chair of Department of Emergency Medicine. “We can take the information we get from clinical patients, and Peter does computer-based simulations. It’s virtual research, if you will, instead of us doing it on a patient where we have to draw your blood, draw your blood, draw your blood. For a department like us, that’s really helpful. We don’t have to create all the research space. We have a collaborative group that can help us test theories before we do them on human subjects.”