As CEO of Community Health Center of Central Missouri, Crystal Sullivan, DO has a clear mission: to foster a culture of preventative care within her clinics.
Sullivan and her staff are furthering that mission through a partnership with a University of Missouri-based program that aims to increase screening rates for one of the biggest cancer killers in Missouri and nationwide: colorectal cancer.
CHCCMO has teamed up with the Missouri Partnership to Increase Colorectal Cancer Screening (MPICCS), a five-year CDC-funded initiative based at the MU School of Medicine to ensure eligible patients are getting screened at their four clinics.
CHCCMO joined the MPICCS program in April 2021 and is already seeing improvement in its screening rate: from January to December 2021, the health system’s colorectal cancer screening rate increased by 10%.
“Our partnership with MPICCS has provided us with the tools and resources to build a long-standing, sustainable colon cancer screening program,” Sullivan said. “In addition, we can use the lessons learned to improve other cancer screening and preventative health care rates.”
CHCCMO’s four clinics are among the 22 rural Federally Qualified Health Center locations statewide that are working with MPICCS to get more of their eligible patients screened.
Partner clinics work directly with MPICCS staff to implement evidence-based interventions. These include using patient and provider reminder systems, providing assessment and feedback to clinicians and connecting patients with financial and transportation resources when needed.
MPICCS practice facilitators work with each clinic to help them improve their screening rates.
“We help practices identify and optimize different procedures within the clinic that can help them keep track of who has and hasn’t been screened,” MPICCS practice facilitator Brandon Spratt said.
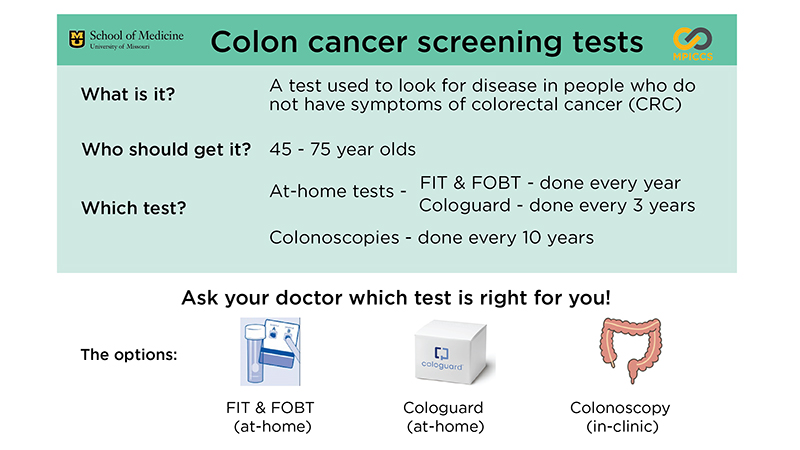
CHCCMO is applying three interventions: a standing order for at-home screening tests, a patient reminder system and quarterly feedback on screening rates for each provider.
Standing orders authorize nurses and other clinic staff to complete a specified clinical task without having to obtain a physician order.
“The standing order empowers our nurses to be able to address colon cancer screening and helps to facilitate a more efficient office visit when the patient is being seen,” Sullivan said.
Patients who have been given at-home screening tests now receive calls from a community health worker to remind them to send completed kits back for analysis. If a patient’s at-home test comes back positive, the community health worker calls to ensure the patient schedules a colonoscopy and connects them with financial or transportation resources if needed.
MPICCS staff create data summaries for each CHCCMO provider that show their individual quarterly screening rate. Each clinician also receives a tangible screening goal — a number of additional patients within their panel that would need to be screened to reach the national screening goal of 80%.
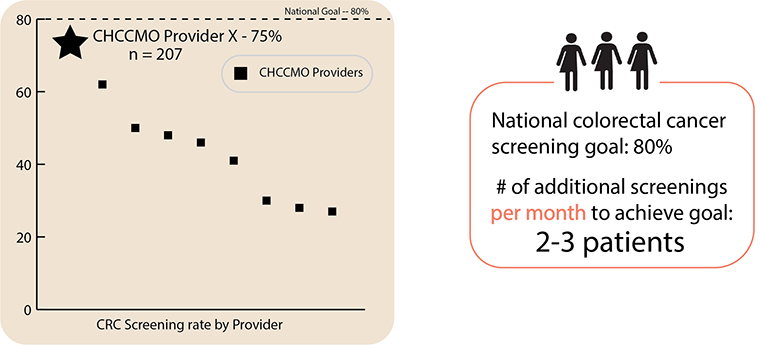
“People might think they are doing a great job with screening, but numbers can be pretty telling,” MPICCS practice facilitator Nuha Wareg said. “When you give them that kind of feedback, you can spark healthy competition among the providers and give them a roadmap with a tangible goal.”
Staff compiles quarterly reports on every clinic’s screening rate and provides the clinics with breakdowns of screening rates by demographic groups like age, race, sex, language used and insurance type.
Partner clinics are applying lessons learned from MPICCS beyond colorectal screenings. Program evaluator Amy Lake has interviewed more than a dozen partners about their MPICCS participation and found that clinics are extending their evidence-based interventions to other preventative health efforts.
“The clinics have realized that these tools can be used for all of the screenings they’re doing,” Lake said. “The program has really gotten people thinking about how to use data in different ways to motivate their providers and clinic staff to do better on screenings.”





